Does Killing Countless Animals Actually Help Treat Alzheimer’s?
What has killing countless animals in Alzheimer’s experiments taught researchers about the disease? Not much.
After decades of wasted time and money, the development of more than 100 unsuccessful drugs, and the loss of an untold number of animals’ lives, no cure for Alzheimer’s disease or method of slowing its progress in humans has been found.
We can and must phase out unreliable tests on animals and replace them with human-relevant, non-animal methods. Read on to find out how.

Here are five things revealed by the overwhelming failure of using animal models for Alzheimer’s research:
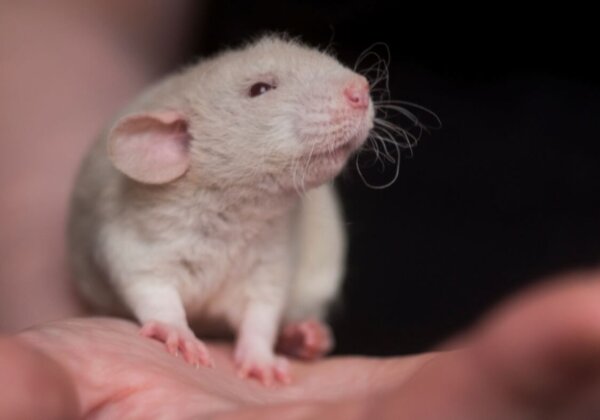
1. Mice, rats, monkeys, dogs, and other animals don’t naturally develop Alzheimer’s disease.
Mice are quick learners and caring parents, and they even sing to their mates. They’re wonderfully complex and interesting. But just because they have thoughts and emotions like humans doesn’t mean we share the same physiology.
Experimenters manipulate the genome of mice and other animals to force amyloid plaques to build up in their brains, just as they build up in the brains of humans with Alzheimer’s disease. While these mutilated animals may have symptoms that resemble those of Alzheimer’s, they don’t actually have the disease.
Studies have shown that trial drugs that remove toxic amyloid-beta protein from animal brains can help these animals. However, the same drugs do not help human patients with memory loss or cognitive problems.
2. Some treatments that have worked in animal trials have actually hurt human patients with Alzheimer’s.
While a compound of drugs known as BACE inhibitors proved successful in tests on mice who’d been genetically altered to develop a pseudo-Alzheimer’s condition, these drugs actually appeared to impair human patients’ cognitive abilities and potentially exacerbate brain shrinkage. Six pharmaceutical companies echoed this same stunning failure.
3. Nearly half a million Alzheimer’s patients need treatments or a cure.
According to the Australian Alzheimer’s Research Foundation (AARF), more than 413,000 Australians have dementia caused by Alzheimer’s disease. It’s estimated that a million Australians will have Alzheimer’s by 2050 unless there’s a significant medical breakthrough. Despite this grave reality, no treatment exists to inhibit the disease’s progression, and the failure rate in humans for new Alzheimer’s drugs is a staggering 99%.
4. Animal testing is archaic and ineffective.
Curing Alzheimer’s requires a 21st century approach. As Allen Institute for Brain Science Senior Investigator Ed Lein stated, “We’re trying to cure a disease of a complex system we fundamentally don’t understand.”
Bradley Hyman, a professor of neurology and Alzheimer’s researcher at Harvard Medical School and Massachusetts General Hospital, expanded on this point, adding that the complexity of Alzheimer’s disease makes it “very difficult to model in experimental systems.” He says, “[D]irect examination of the human brain is without a doubt crucial to understanding the disease.”

5. We must stop killing animals and actually focus on the human brain.
More than ever, researchers must embrace non-animal research methods that are actually relevant to human physiology.
Australia has long been a leader in Alzheimer’s disease research using non-animal methods. For example, in2012, the Medical Advances Without Animals Trust funded research undertaken at the University of Wollongong aimed at the development of non-animal cell systems to create drugs for treating Alzheimer’s disease in order to replace the use of mouse neurons with induced pluripotent stem cells from Alzheimer’s patients.
Today, research continues, and although Australian charities such as the AARF and the Dementia Australia Research Foundation continue to fund experiments on animals, we applaud the not-for-profits that support various human-based research projects.
These range broadly from studying molecular mechanisms underlying Alzheimer’s disease in cultured human cells and human mini-brains (brain organoids) to using artificial intelligence, developing detection and screening tools aimed at improving the diagnosis and treatment of Alzheimer’s disease, and finding methods for prevention and early intervention, with a focus on adjusting critical lifestyle factors such as sleep or exercise.
What You Can Do
Support charities that actually help humans and don’t test on animals. Humans and other animals deserve better from experimenters than death and failure.
Read up on the Research Modernisation Deal – a PETA affiliate’s strategy for phasing out unreliable, cruel tests on animals and moving towards ethical, non-animal methods – and share what you learn with your friends and family.